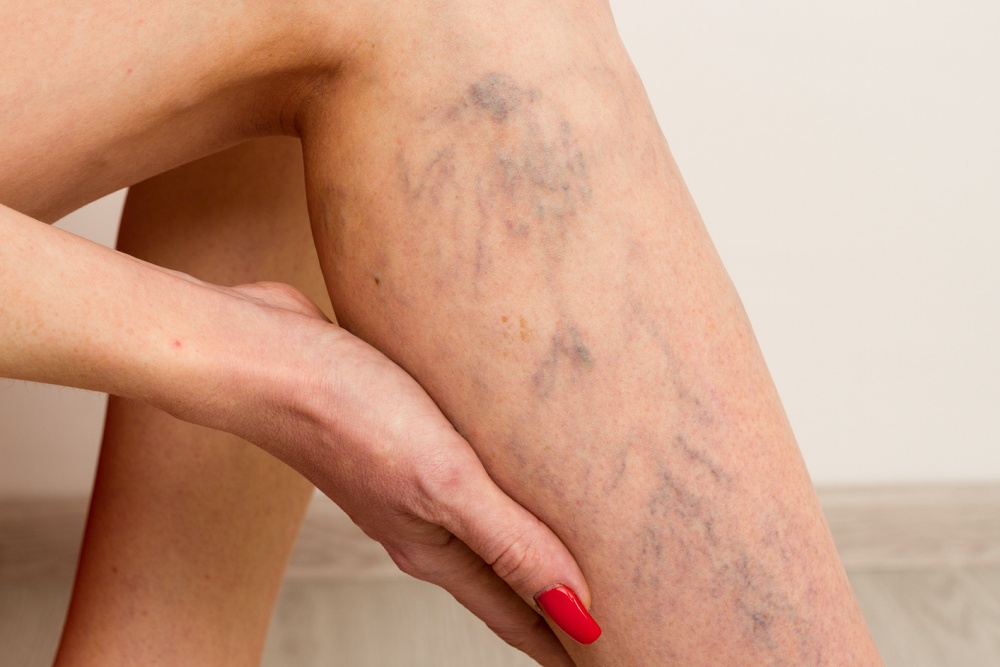
Veins are a part of the body’s circulatory system, responsible for returning deoxygenated blood to the heart. The valves within these veins can sometimes weaken or become damaged. This damage may cause blood to pool, leading to the development of swollen, enlarged, and twisted veins known as varicose veins.
What Are Varicose Veins?
Arteries carry blood from your heart to your tissues, and veins return it to your heart for recirculation. To return blood to your heart, the veins in your legs must work against gravity. Tiny valves in your veins open as blood flows toward your heart, then close to stop blood from flowing backward.
When these valves fail to function properly, blood can flow backward and pool in the veins. This causes the veins to stretch or twist, leading to the visible and sometimes uncomfortable condition of varicose veins. Factors that may increase the likelihood of developing them include age, family history, gender, pregnancy, and prolonged periods of standing or sitting.
What Are the Types?
These veins are categorized based on their size, appearance, and location. Medical professionals classify them into several distinct types. A medical professional can determine the appropriate management approach.
Saphenous Varicose Veins
The great saphenous vein (GSV) and the small saphenous vein (SSV) are the two main superficial veins in the legs. When the valves within these large veins fail, they can become varicose. Saphenous varicose veins are large, bulging, rope-like veins that are often visible beneath the skin.
Spider Veins
Spider veins are the smallest type of visible veins. They are fine, web-like lines that can be red, blue, or purple. These veins lie very close to the skin’s surface and may appear on the legs or face. Spider veins are typically asymptomatic, meaning they do not usually cause pain or other physical symptoms, but they can be a cosmetic concern for many individuals.
How Are They Treated?
The treatment for varicose veins depends on the type, severity of symptoms, and the individual’s overall health. A vein specialist can perform a physical examination. They may use diagnostic tools like an ultrasound to evaluate vein function and determine the extent of the condition.
Initial management often involves self-care measures. These can include elevating the legs, engaging in regular exercise to improve circulation, and wearing compression stockings. Compression stockings apply gentle pressure to the legs, which assists the veins and leg muscles in moving blood more efficiently.
For veins that do not respond to conservative measures or for cosmetic purposes, several minimally invasive procedures are available. Sclerotherapy involves injecting a solution directly into the vein, causing it to scar and collapse. Endovenous thermal ablation uses laser or radiofrequency energy to heat and seal the affected vein.
Seek Professional Vein Treatment
Modern medical advancements offer a range of effective and minimally invasive options to address them. Consulting with a qualified vein specialist is a proactive step toward understanding your specific condition and exploring the available treatment paths. A specialist can provide a thorough diagnosis, explain the underlying causes of your varicose veins, and recommend a personalized treatment plan designed to restore comfort and improve vein health.